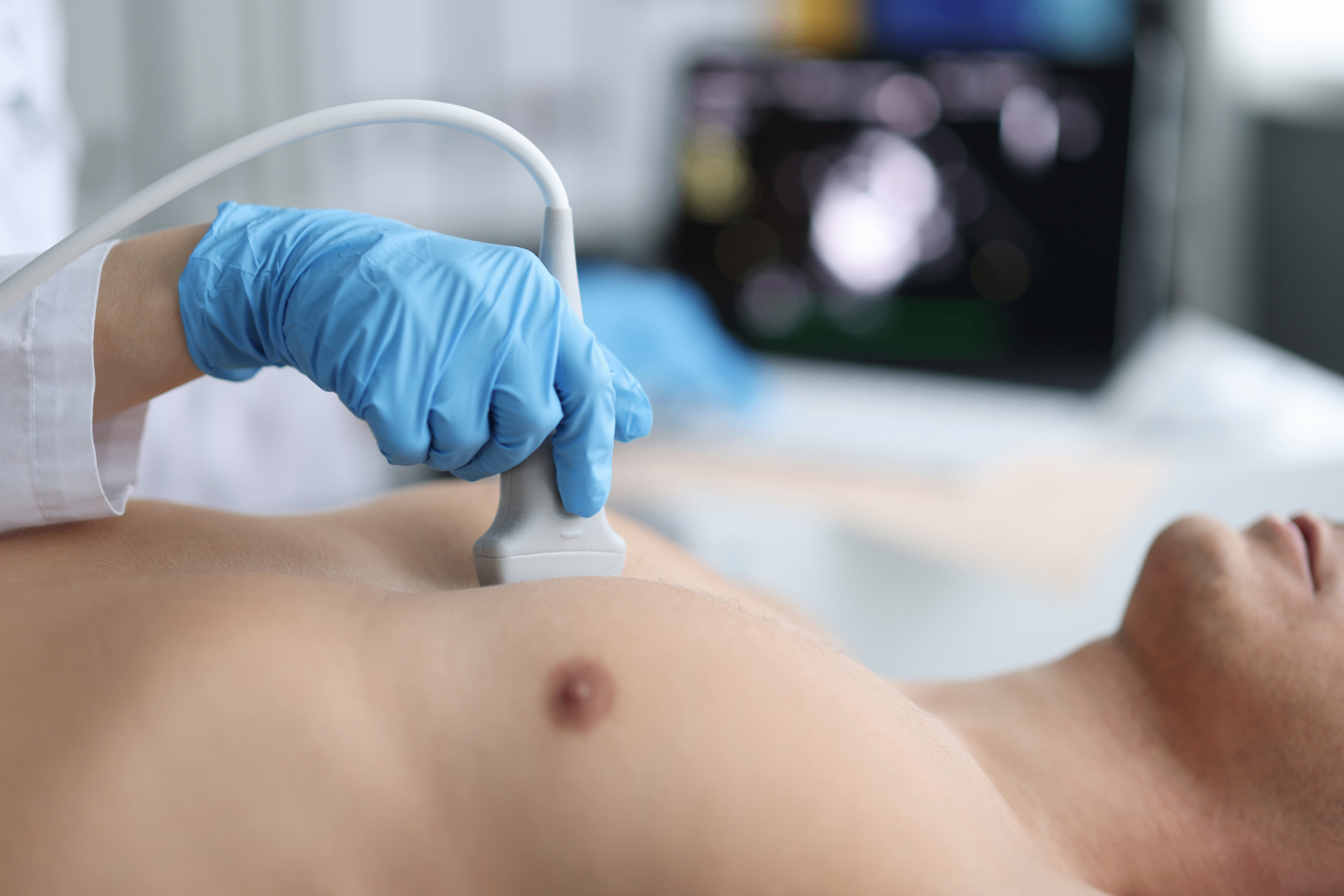
Additional tests
Disclaimer: The following information is for educational purposes only and is not intended as medical advice. Always consult with a healthcare professional for medical advice and treatment.
Based on the results of previously conducted imaging and/or tissue examinations, additional supplementary investigations may be considered.
Sputum is mucus mixed with saliva that is coughed up from the deep airways during a respiratory infection. This mucus is examined under the microscope for the presence of lung cancer cells.

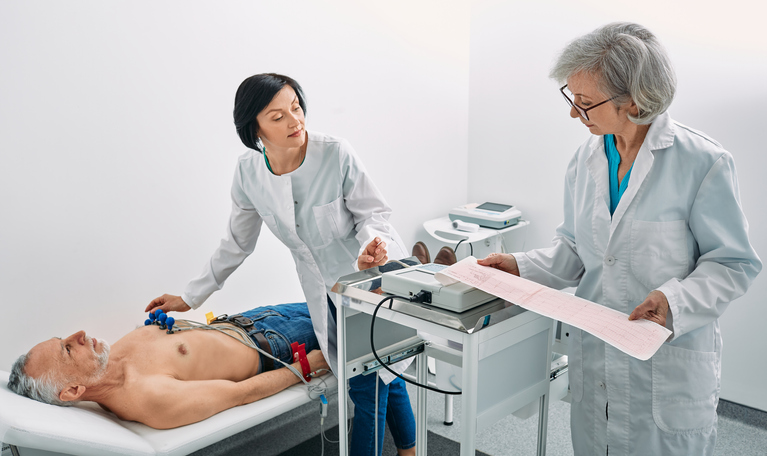
An ECG, or electrocardiogram, monitors heart function (rhythm, frequency, and potential abnormalities).

A lung perfusion-ventilation scan visualizes blood flow (perfusion) and air distribution (ventilation) in the lungs. For this examination, a tracer — a mildly radioactive substance — is injected into the arm vein, and a small amount of air with harmless and odorless mildly radioactive gas is inhaled. The scan images then show how blood flows through the lungs and how air distributes. The goal of this examination is to determine the extent to which the tumor(s) have affected lung tissue and can give more information if a pneumectomy (removal) of the lung is possible.
A bone scan creates images of the skeleton to study bone metabolism and detect lung cancer metastases. The bone scan operates on the same principle as a PET scan. Prior to the scan, a tracer is injected — in this case, a small amount of mildly radioactive substance called EDP or MDP (diphosphonate) that attaches to the micro-architecture of the bones, especially in areas with increased metabolism, such as metastases. These areas become visible on the scan.

In a lung puncture or transthoracic puncture, a thin hollow needle is inserted from the outside through the chest wall into the lungs to extract a small piece of lung tissue for examination. This technique is used when the tumor or metastases are not easily accessible with bronchoscopy.
The lungs are surrounded by two membranes called the visceral pleura and the parietal pleura. There is always a small amount of fluid, pleural fluid, in the space between these membranes. When lung cancer has spread to the pleura, more fluid is produced, and less is drained, causing the accumulation of pleural fluid (pleural effusion) or other abnormal cells such as white blood cells, red blood cells, etc.
A mediastinoscopy examines the mediastinum, the space between the lungs in the middle of the chest, to check for metastases in the lymph nodes around the lungs. A mediastinoscope is inserted through a small incision in the chest wall just above the sternum. A mediastinoscope is a specialized type of endoscope. During the examination, fluid or tissue samples can be taken from the lymph node(s) using the mediastinoscope for analysis. A mediastinoscopy is typically performed if the results of endoscopic ultrasound (EUS and EBUS) were not clear enough or if the lymph nodes in the mediastinum could not be accessed otherwise.
In a thoracoscopy or pleuroscopy, the pleural cavity, the small space between the chest wall and the lung, is examined using a thoracoscope, a specialized type of endoscope. The thoracoscope is inserted through a small incision in the chest wall between the ribs, allowing examination of the pleural cavity. Thoracoscopy is often performed to take a piece of lung or pleura tissue for further analysis.
